OBGYN - Normal and Abnormal Labor
From Iusmicm
Revision as of 22:14, 14 December 2011 by 134.68.138.157 (Talk)
Labor: Normal, Abnormal, and Points Between
Definitions
- Labor: regular / rhythmic contractions, cervical dilation and effacement.
- Must have cervical change to call it labor.
- Dilation: cervix develops a wider opening.
- Effacement: becomes shorter.
- Labor is considered "preterm" if it commences before 37 weeks EGA (estimated gestational age)
- 10-12% of pregnancies include preterm labor.
- Labor is considered "postdates" if it commences after 42 weeks EGA.
- Braxton Hicks contractions are contractions of a weak or irregular nature.
Physiology of Labor
- There are many factors that play a role in the coordinated contraction of all the uterine smooth muscle for labor.
- Progesterone and Relaxin are key regulating factors in animals.
- Relaxin does not play a role in humans.
- When 17 alpha-hydroxyprogesterone caproate is given, we see fewer preterm contractions so we know progesterone plays a role but we don't see it physiologically.
- Progesterone levels don't drop until after the placenta is delivered.
- Gap juctions of the uterine smooth muscle are increased near term.
- Presumably to augment myofiber-myofiber communication for a well sequenced contraction.
- Allow easy ability for electrical potential to cross.
- Oxytocin, surprisingly, shows no change in blood levels but there are increased number of oxytocin receptors.
- Oxytocin receptors, however are elevated.
- Oxytocin does promote the influx of calcium ions (and therefore increased contractions).
- There is a paracrine oxytocin production from the dicidual and placenta with subsequent increase in receptors in the myometrium.
- Made in the posterior pituitary.
- Several prostaglandins are elevated for labor: PGE1, PGE2, PGF2alpha
- Makes collagenase to help break down collagen of the cervix to allow dilation and effacement.
- Mother becomes more sensitive to changes in Ca at term.
- This is presumably because the uterine muscle is storing up more and more Ca to augment contraction.
- Like prostaglandins, many cytokines are elevated: IL-1, IL-6, IL-8, TNF-alpha.
- Intermediate reactions in the labor pathway.
- Infections can sometimes induce these types of cytokines and thus induce labor.
- NO is another intermediate reactor.
Labor and Delivery Admission
- The workup for a L&D admission includes:
- H&P:
- Fetal monitoring
- Leopold’s maneuver
- Vaginal exam
- R/o (rule out) placenta previa and ROM first
- Cervical dilation / effacement / station and fetal position
- H&P:
Fetal Monitoring
- With fetal monitoring we are concerned with the baby's heart rate and the uterine pressure.
- There are several technical methods for fetal monitoring.
- We can monitor externally via ultrasound and pressure transducers.
- We can monitor internally (if the membranes are ruptured) by putting a pressure transducer into the uterine cavity.
- A clip on the baby's scalp can mark each R wave.
Fetal Monitoring - Normals
- For baby's heart rate, the baseline should be around 110-160 bpm.
- We are looking for: variability, accelerations / decelerations
- For uterine pressure (contractions) we are looking for: frequency, duration, uterine tone.
- Tone is important because the baby gets better blood flow when the uterus is resting.
Variability and Accelerations / Decelerations
- Variability:
- Absent: 0-2 bpm
- Start worrying about fetal acidosis.
- Fix the environment or get the baby out.
- Minimal: 3-5 bpm
- Moderate: 6-25 bpm (ideal).
- Marked: saltatory, >25 bpm
- Absent: 0-2 bpm
- Fetal Monitoring:
- Good, classic accelerations go up by 15 beats per minute and last for 15 seconds.
- If the pregnancy is less than 34 weeks, "10x10" is acceptable.
Decelerations
- Early declerations: occur with cntx
- Start and end with the contraction
- Non worrisome
- Head compression leads to vagal stimulation at the posterior fontanelle
- Recall that vagus carries parasympathetics to the heart
- Late decelerations: begin at peak of cntx or after
- Fetal hypoxia is usually the culprit of late decelerations.
- Occurs due to chemoreceptors in the carotid arch that sense the decreased pO2 leading to vasoconstriction and then bradycardia
- Variable: can occur at any time
- Variable decelerations should raise one's suspicion for cord compression
- Variable Decelerations: mild, moderate, and severe.
- Lower the blood pressure the more severe.
- Longer the duration the more severe.
- Severity of variable decelerations are a function of blood pressure and duration
Categories of Heart Tracings
- Category 1:
- Baseline rate: 110-160 bpm
- Baseline FHR variability is moderate
- Accelerations: present or absent
- Late or variable decelerations absent
- Early decelerations present or absent
- Category 2:
- Everything not in 1 or 3
- Category 3:
- Absent baseline variability (recall, a sign of acidosis)
- Recurrent late decelerations
- Recurrent variable decelerations
- Bradycardia
- Sinusoidal pattern (a sign of fetal hypoxia with severe anemia; think Rh disease)
Fetal Lie, Presentation, Attitude, and Position
- Clinical: abdomenal palpation, auscultation of fht’s, vaginal exam
- Studies: u/s, x-ray, MRI
- These are done very rarely as we can determine the lie and presentation rather easily via physical examination.
Definitions
- Lie: relation of long axis of fetus to long axis of mother.
- Longitudinal
- Transverse
- Oblique
- Presentation: part of baby foremost in the pelvis
- Cephalic
- Breech (bottom)
- Shoulder
- Face
- Compound:
- Head / hand -> watch (usually resolves itself; may apply a noxious stimuli to the hand)
- Head / foot-> c-section (will not resolve itself; requires c/s)
- Cord prolapse (funic presentation): an emergency.
- When the cord drops into the vagina.
- Must move quickly to c/s.
- Attitude: how the baby presents its head
- Normal attitude is folded on itself w/ flexed head
- Position: relation of presenting part to maternal pelvis anterior aspect
- When the baby presents cephalically, the reference point on the baby to be referenced to the anterior pubis of the mother is the occiput
- When the baby presents facially, the reference point is the mentum
- When the baby presents as a breech, the reference point is the sacrum
- When the baby presents transverse (shoulder), the reference point is the acromion process
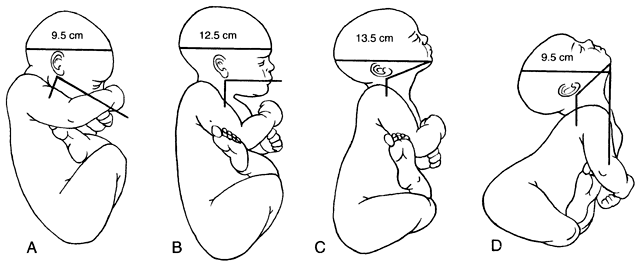
Fetal Attitude
- There are a variety of ways the fetus can present at the os; these are called attitudes:
- Full flexion (A)
- Normal, smallest diameter.
- Military attitude (B)
- Brow presentation (C)
- Face presentation (D)
- Full flexion (A)
- Leopold’s Maneuver can be used to determine the attitude of the fetus.
- First maneuver: what is occupying the fundus?
- Soft like a butt or hard like a head?
- Second maneuver: on which side is the fetal spine?
- Third maneuver: what is presenting at the pelvis?
- Soft like a butt or hard like a head?
- Fourth maneuver: what is the attitude, based on the flexion / extension of the head?
- First maneuver: what is occupying the fundus?
- Can correlate with CT if there is any questions.

Vaginal Exam
- We are trying to determine if the cervix is starting to dilate or efface.
- We describe effacement as a percent of normal length:
- Normal length of a cervix is 4cm.
- So if the cervix is observed as being 2 cm effaced, we call it 50%.
- Station: the lowest point of the fetus in reference to the ischial spines.
- The stating is described as -1 (and so on, for every centimeter) it is above the ischial spines.
- The station is described as +1 (and so on, for every centimeter) it is below the ischial spines.
- Position:
- Most common is cephalic.
- Use the occiput as the baby reference point when describing position against the maternal anterior pubis.
- "right" and "left" shifts describe maternal right and left
- To determine which aspect is the occiput, recall there are ant and post fontanelles (along which to orient) and the frontal suture (to identify the anterior aspect of the baby).
- Pelvimetry:
- Performed at the first pre-natal visit and upon admission for L&D.
- Describes adequacy of the pelvis for baby delivery.
- Measures pelvic inlet, the midpelvis, and the pelvic outlet.
Pelvic Inlet
- True pelvic inlet measurement is from superior pubic ramus to the sacral prominence.
- However, this can't be measured directly so we measure it indirectly.
- True conjugate is also called the obstetric conjugate.
- The diagonal conjugate is measured with one's third finger, along toward the thumb.
- True obstetric conjugate = diagonal conjugate – 1.5 to 2.0 cm
- Diagonal conjugate: >11.5 cm is adequate
Midpelvis
- Sacrum – hallow versus shallow (flat):
- Hallow is concave like a bowl of soup and gives more room for baby moving.
- Ischial spines – blunt vs. prominent
- blunt is better; more room
- Pelvic sidewalls
- Parallel = OK
- Divergent = good
- Convergent = bad
Pelvic Outlet
- Bituberous diameter:
- > 6-8 cm is good
- Measured by placing fist up against the butt.
- Pubic arch:
- > 90 degrees is good
Stages of Labor
- 1st Stage: beginning of cervical dilation to complete dilation (10 cm)
- 2nd Stage: complete dilation to delivery of fetus
- 3rd Stage: delivery of placenta
- up to 30 minutes
- 4th Stage: first hour after delivery of placenta
- Big fluid shift, high risk of post-partum hemorrhage.
- Monitoring mom for vitals
- Monitoring firmness of uterus (should remain firm to inhibit hemorrhage by pressing layers of endometrium together)
Cardinal Movements of Labor=
- Engagement
- Flexion (of the head)
- Descent
- Internal rotation
- Extension
- External rotation
- Expulsion
- If the face is anterior, it can still extend.
- If mentum-posterior, there can be no extension, so it cannot deliver.
Labor Curve
- The first phase of minimal cervical change is latent phase.
- Minutes, hours, days!
- Active phase
- > 1 cm change / hour
- Baby will move from -5cm station to 0 to +5 as it delivers.
Prolonged / Arrested Labor
- When labor isn't moving along, consider your 3 Ps
- Power: uterine contractions
- Are they strong enough?
- Give oxytocin?
- Pelvis: adequate?
- Do your pelvimetry to make sure pathway is sufficient
- Passenger: EFW, position / attitude
- Is the baby too big?
- Is the position wrong? (occiput posterior)
- Is the attitude wrong? (military)
Dysfunctional Labor
| Pattern | Nullip | Multip | Rx | ||||
|---|---|---|---|---|---|---|---|
| Prolonged latent phase | >20 hr | >14 hr | Rest, AROM (augmented rupture of membranes; helps augment maternal environment for labor), Pitocin (oxytocin) | ||||
| Protracted dilation | <1.2 cm/hr | <1.5 cm/hr | AROM, Pit | ||||
| Protracted descent | <1 cm/hr | <2 cm/hr | Pit | Arrest of dilation | >2 hr | >2 hr | AROM, Pit, C/S |
| Arrest of descent | >2 hr | >1 hr | Vacuum, forceps, C/S |
Cesarean Section
- History
- Caedere -> caesura: to cut; seco: to cut.
- "Cut Cut"
- Francois Rousset (1581)
- First reported case with survival.
- Questionable
- Max Sanger (1882)- Leipzig
- Work on the American frontier
- Sewed the womb shut! (Whoa!)
- Crazy b/c the womb was considered an awful, evil thing, that shouldn't be sewn shut b/c all those bad humors would stay inside!
- Most common surgical procedure
- 1965: <5%, 1996: 20.7%, 2004: 29.1%
- No change in cerebral palsy rate
C-section - Techniques
- Uterine Incisions
- Low transverse
- The most common way because it runs with the grain of the muscular fibers.
- Also, this area does less labor contracting so next pregnancy is less likely to result in rupture.
- Low verticle
- Classical
- Kerr
C-section - Indications
Fetal C-section Indications
- Distress / intolerance of labor
- FHT of category 2 or 3
- Malpresentation (breech, transverse)
- Twins, multiples
- Vertex / Vertex = allow to labor
- Some congenital anomalies
- NTD
Maternal-Fetal C-section Indications
- Arrest of active labor
- Pretty common
- Failed induction of labor (?)
- Placenta previa, vasa previa
- When the placenta covers the cervical os.
- When the placental vessels course between baby and os.
- 50% mortality post-rupture!
- Active HSV outbreak
- HIV+ (viral load >1000/ml)
- If mom is on ARV therapy, there is no decrease in transmission with c/s.
- EFW > 4500 - 5000 grams (increasing risk of shoulder dystocia)
- Use u/s to estimate weight.
Maternal C-section Indications
- Obstructive tumors (some leiomyomas)
- Severe condylomata acuminata
- Cervical cancer
- Abdominal cerclage
- Prior c-section
- Risk of uterine rupture is 0.5-1%
- Can be catastrophic
- Prior vaginal colporrhaphy
- Vaginal delivery contraindicated medically
- Pregnant???
- No!
C-section - Risks
- At time of surgery / Immediate post-op
- Infection: endometritis, wound infection, septic pelvic thrombophlebitis (SPT)
- Bleeding: transfusion, hysterectomy
- Damage to fetus
- Very small; no larger than with vaginal delivery.
- Damage to adjacent organs
- Subsequent pregnancy:
- Adhesions
- Uterine rupture
- Placenta previa (when the placenta covers the os) may convert to accreta (when the placenta invades the myometrium).
- Accreta carries huge risks because there is often massive bleeding.
- Accreta puts the mother a risk of death.
- That is, placenta previa with a previous c/s has a very high risk of being bad!
- 0 –> 5% (number of previous c/s, risk of accreta given a placenta previa)
- 1 –> 24%
- 2 –> 48%
- 3 –> 67%
There will be a test question on prior c/s and placenta previa.
Operative Vaginal Delivery
- Forceps and vacuum can be used to guide the baby's head out of the pelvis.
- There are many different types and procedures.
Operative Vaginal Delivery - Classification
- We want, first, to be sure the baby has reached the pelvic inlet.
- Didn't talk about any of this:
- Outlet: scalp visible at introitus w/out separating labia; no rotation
- Low: leading point of skull at or below +2 cm station
- Rotate < 45°
- Rotate > 45°
- Mid: above +2 cm station but engaged
Operative Vaginal Delivery - Indications
- Nonreassuring FHT’s
- Prolonged 2nd stage of labor
- Shortened 2nd stage if pushing / Valsalva not indicated
- Maternal exhaustion
Operative Vaginal Delivery - Prerequisites
- Cervix completely dilated
- Ruptured membranes
- Fetal skull engaged in pelvis
- Empty bladder
- Position! Position! Position!
- Before we put anything on the baby's head, we have to know the position so we don't break the nasal bone or deform the child.
- Adequate pelvis
- Adequate anesthesia
Operative Vaginal Delivery - Forceps Assisted
- Use the same angles when applying traction.
- Apply the extension just like in a non-operative vaginal delivery.
Operative Vaginal Delivery - Risks
- Maternal:
- Vaginal / perineal trauma, damage to rectal sphincter
- Mostly forceps issues with mom
- Fetal:
- Mostly vacuum issues with baby
- Cephalohematoma
- Subgaleal hemorrhage
- Bony facial trauma
- Facial nerve injury
- Intraventricular hemorrhage
Birth Trauma
- Caput succedaneum:
- Very common
- Crosses midline
- Subgaleal hemorrhage:
- Does not cross midline
- Rare
- Hypovolemia and DIC
Common Post Partum Problems
- PP Hemorrhage: >500cc (>1000cc for c/s):
- Atony
- When the uterus won't contract.
- Linings aren't collapsed together to stop bleeding.
- Lacerations (cervix, vagina, perineum)
- Retained placenta
- Keeps the endometrium layers from coapting (collapsing together).
- Uterine rupture
- Uterine inversion
- Amniotic fluid embolism
- Atony
- Endometritis:
- Fundal tenderness w/ temperature >38°C x 2 or >38.5°C
- Polymicrobial infection
- More common after c/s
- Prolonged ruptured membranes
- Chorioamnionitis
- Treat with broad spectrum antibiotics
PP / Post-Op Fever
- Causes and symptoms
- Wind (atelectasis, pneumonia)
- Wound (seroma, necrotizing fasciitis)
- Water (UTI)
- Walk (thrmobophlebitis)
- Wonder drug (drug reaction)
- Womb (endometriosis)
- Wean (mastitis, engorgement)
