Exam 1 Physical Diagnosis Objectives
From Iusmicm
(Difference between revisions)
| Line 310: | Line 310: | ||
# Clinically correlate the symptoms and physical exam findings pertaining to the nose for the following disease processes: allergic rhinitis, sinusitis, and nonallergic rhinitis. | # Clinically correlate the symptoms and physical exam findings pertaining to the nose for the following disease processes: allergic rhinitis, sinusitis, and nonallergic rhinitis. | ||
# Generate a diagnosis and/or differential diagnosis based on symptoms and/or physical exam findings of the nose. | # Generate a diagnosis and/or differential diagnosis based on symptoms and/or physical exam findings of the nose. | ||
| + | |||
| + | |||
| + | |||
| + | |||
| + | ===Chapter 12=== | ||
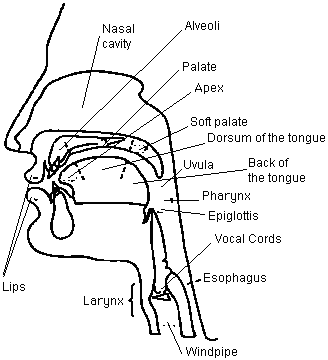
| + | *Know the structures of the oral cavity and pharynx. | ||
| + | **http://media-3.web.britannica.com/eb-media/91/74891-004-345232AC.jpg | ||
| + | **http://4.bp.blogspot.com/_hL0QrZsPcvY/SaP_z9urWaI/AAAAAAAAAYM/Djf9xDzyaes/s400/or4.gif | ||
| + | |||
| + | *Know the functions of the pharynx. | ||
| + | **Subdivisions: nasopharynx, oropharynx, hypopharynx. | ||
| + | **Fxn: provides swallowing, speech, and an airway. | ||
| + | |||
| + | *Know the important symptoms of disease of the oral cavity. | ||
| + | **Ulceration, bleeding, mass, halitosis, xerostomia (dry mouth). | ||
| + | |||
| + | *Apply the components of the physical exam of the oral cavity and pharynx to a patient. | ||
| + | **See cd. | ||
| + | |||
| + | *Clinically correlate the signs and symptoms of the following conditions: | ||
| + | **Aphthous ulcer | ||
| + | ***Single canker sore. Most common acute oral ulcer. | ||
| + | ***Relatively superficial w/ raised borders. On buccal or labial mucosa. | ||
| + | **Herpetic ulcer | ||
| + | ***acute multiple ulcers, associated w/ vesicles. | ||
| + | ***On mucocutaneous junction, hard palate, or gingivae. | ||
| + | ***Crusting when bullae break. | ||
| + | **Chancre | ||
| + | ***Painless, single lesion on lips or tongue. | ||
| + | ***Lesion w/o central necrotic material. | ||
| + | ***May have tender lymphadenitis. | ||
| + | **Squamous cell carcinoma: | ||
| + | ***Single indurated sore on lips, tongue, mouth floor, or tongue (esp. on lateral borders) | ||
| + | ***Erythroplakia of mouth floor and soft palate. | ||
| + | ***Raised border, absence of necrotic material in crater. | ||
| + | ***May have painless lymphadenopathy in neck. | ||
| + | **Candidiasis | ||
| + | ***Burning tongue, inside of cheek or throat. | ||
| + | ***Whitish pseudomembrane. | ||
| + | ***Peeled off to reveal raw, red area that may bleed. | ||
| + | **Erythroplakia | ||
| + | ***Painless, red area. | ||
| + | ***Granular, red papules that bleed. | ||
| + | **Leukoplakia | ||
| + | ***Painless, white area. | ||
| + | ***Hyperkeratinized. Can’t be scraped off. | ||
| + | ***Looks like flaking white paint. Often speckled w/ red spots. | ||
| + | ***If associated with adenopathy, could be malignancy. | ||
| + | **Lipoma | ||
| + | ***Painless mass on inner surface of cheek or tongue. | ||
| + | ***Yellowish, soft, freely mobile. | ||
| + | **Lichen planus | ||
| + | ***Usually no symptoms. | ||
| + | ***Erosive form causes burning sores on inner cheeks and tongue. | ||
| + | ***White reticulated papules bilaterally in lace-like pattern. | ||
| + | ***Erosive form is hemorrhagic, ulcerated w/ possible white areas or bullae. | ||
| + | ***May have pseudomembrane covering. | ||
| + | **Mucocele | ||
| + | ***Intermittent painless swelling of lower lip, or inside cheek. | ||
| + | ***Slightly bluish. | ||
| + | ***Dome-shaped, freely-mobile cystic lesion. | ||
| + | **Hairy Tongue | ||
| + | ***Gagging sensation. | ||
| + | ***Large brown or black painless lesion on top of tongue. | ||
| + | ***Elongation of filiform papillae and color change. | ||
| + | |||
===Chapter 13=== | ===Chapter 13=== | ||
Revision as of 21:35, 28 September 2011
- Note, much borrowed from generous, previous IUSM medical students.
Contents |
Chapter 1
- Apply the guidelines for using a medical interpreter when a medical interpreter is needed for a patient interview.
- need to be trained in med. Terminology
- same sex and age as patient
- establish an approach with interpreter before talking to patient
- speak and look at patient
- do not expect word for word translation
- ask interpreter about patient fears and expectations
- use short questions
- use simple language
- keep explanations brief
- avoid using "if", "would" and "could" questions and statements
- avoid idiomatic expressions
- Define the “rule of 5 vowels” and use the 5 vowels in a patient interview.
- AEIOU: audition, evaluation, inquiry, observation, understanding
- audition: listen to story
- evaluation: determine what is relevant
- inquiry: ask appropriate questions
- observation: importance of non-verbal communication
- understanding: show empathy and signs that you understand and care
- Recognize the difference between a “symptom” and a “sign”.
- A symptom is what a pt feels.
- A sign is what a physician detects.
- Select the appropriate terminology and questions to begin a medical interview.
- Greet with your name, ask their name, make eye contact, shake hands, smile, state your purpose and intent.
- Apply the use of open-ended questions when conducting a medial interview.
- Start with open ended questions, focus down with direct questions.
- Apply the use of direct questions when conducting a patient interview.
- ROS should be demarked with a transition statement explaining that you're not looking for simple yes or no answers.
- Follow positive ROS responses with open ended and OPQRST questions.
- Discriminate patient symptoms using the O-P-Q-R-S-T mnemonic.
- OPQRST:
- onset (time, activity);
- provoke / palliate (what makes it worse or better);
- quality (characteristics like blurry, sharp, burning, deep, etc.);
- radiation (does the symptom occur anywhere else or associate with any other symptom);
- severity (1-10);
- timeline
- CLOSER:
- characteristics (quality, severity)
- location (and radiation)
- onset (and duration)
- symptoms associated
- exacerbating factors
- relieving factors
- OPQRST:
- Discriminate which questions to avoid and not use when interviewing a patient.
- Avoid rapid-fire questions; "have you lost or gained weight or had any nausea or vomitting?"
- Avoid medical jargon; "where you tachypnic when the pain started?"
- Avoid leading or biased questions; "you don't have any heart problems do you?"
- Describe the parts of the medical history and include each part when writing a medical history.
- Chief complaint
- History of Present Illness
- Past Medical History
- Social History
- Family History
- Psychosocial and Spiritual History
- Sexual and Reproductive History
- Review of Systems
Chapter 2
- Describe the various responses to illness in a patient.
- There are several major responses to illness, including: anxiety, depression, denial, projection, and regression.
- Anxiety: characterized by uneasiness and a sense of impending danger
- Depression: a chronic state of lowered mood
- The most common reaction to illness and perhaps the most overlooked.
- 20% of pts with major illnesses express depression (especially cancer pts).
- Noted by brief answers, slow speech, and low volume.
- Thoughts are negative, with lots of (perceived) inadequacy, defeat, and worthlessness.
- Denial: acting and thinking a part of reality is not true.
- Recall that denial is a defense mechanism used to guard against an inner tension that causes anxiety. Denial prevents the turmoil from producing overt anxiety.
- The more acute the illness, the less room for denial; the more insidious the illness, the more denial.
- May need to interview a reliable informant when denial is so severe accurate answers cannot be secured.
- Projection: perceiving one's own emotions in another being
- Recall that projection is a defense mechanism that guards against an inner tension and manifests as the pt perceiving their own emotion in the interviewer (fear, anger, for example).
- A danger for the Doctor-Pt relationship.
- Regression: an unconscious return to an earlier stage of physical or emotional development in which the pt was free from the demands of disease and was often gratified.
- Regression is a defense mechanism.
- Describe the variety of patient types and how to approach them during an interview.
- Silent
- Characteristics: shy, insecure, easily embarrassed normally or silent from fear of illness. May be depressed.
- Approach: Use directed questions, not open-ended.
- Over-talkative
- Characteristics:
- Approach: use courteous interruption followed by another direct question. Avoid open-ended questions.
- Seductive:
- Characteristics: many have personality disorder and have fantasy of intimacy with doctor.
- Approach: Keep empathy and reassurance to minimum. Keep professional distance.
- Angry
- Approach: Realize reactions are to illness and not personal. Confront about anger and allow to vent, proceed slow, avoid interpretations and ask questions about present illness.
- Paranoid
- Characteristics: Reassurance tends to be threatening.
- Approach: Complete questioning and don’t try to convince about false ideations. Avoid any anger.
- Insatiable
- Character: never satisfied.
- Approach: Handle with firm, noncondescending approach. Use definite closing statement.
- Ingratiating
- Character: attempts to please interviewer.
- Approach: Try to give “right” answer. Stress importance of accuracy
- Aggressive
- Character: often has personality disorder, easily irritated and can fly into rage.
- Approach: Stay away from provoking anxiety early and establish rapport.
- Help-rejecting
- Character: seen many experts and no one can figure out what is wrong. Return saying suggestions didn’t work. New symptoms appear after one goes away. Blame “illness” for disappointments.
- Approach: Use strong emotional support and gentile reasoning
- Demanding
- Character: Use intimidation and guilt to force others to take care of them. See self as neglected, may have outburst of anger and have power struggle with doctor.
- Approach: Provide firm boundaries, elicit and set clear expectations.
- Compulsive
- Character: concerned about every detail, use projection
- Approach: Provide detailed and specific info in a straight forward way
- Dependent
- Character: finds life hard without help. Need to care for closely, but they can take advantage of doctors by demanding time.
- Approach: Be direct about limits without leaving rejected.
- Masochistic
- Character: go thru life suffering mentally, but don’t seek physical abuse or pain. Feel they self-sacrifice and handle illness well, but may feel threatened by recovery.
- Approach: Don’t promise cures, attend to all aspects of illness.
- Borderline
- Character: personality disorder with instability, splitting, impulsiveness and unstable moods. Are always afraid, but may mask with anger.
- Approach: Use lots of reassuring words.
- Silent
- Describe how disease can influence the type of patient response.
- Disabled
- Theme is mistrust of healthcare; response is assurance.
- Sort out emotional problems for physical ones.
- Smile and nice words help them cooperate.
- Don’t like their routines changed.
- If hearing impaired sit in front so they can read your lips or speak louder, write things down if needed.
- If vision impaired: occasionally touch patient’s arm so they know where you are. Avoid non-verbals.
- Developmentally delayed need guardian to give history.
- Cancer
- -5 major concerns: loss of control, pain, alienation, mutilation and mortality.
- Doctor may be afraid of patient’s questions about death and patient feels rejected.
- Doctor needs to recognize their limitations.
- Allow patient to vent and promote dialogue.
- AIDS
- Fearful for life and being stigmatized which may result in delay of seeking care.
- Denial is important and may fear doctors.
- Fear worsened by anxiety of health care workers who care for them.
- Unsympathetic rejection of AIDS patients leading to anxiety, hostility and depression.
- Be supportive with out false sense of hope.
- Give facts and make sure staff is educated.
- Dyphasic
- Impairment of speech and can’t arrange words correctly.
- Always assume patient is aware if talking with them in the room.
- Give patient pen and paper and or ask yes / no questions.
- Psychotic
- Impaired reality testing abilities and can’t communicate effectively.
- May have hallucinations and delusions.
- Remain calm and get assistance if violent episode.
- May have Munchausen’s and be malingerers.
- Many self injure.
- Demented or Delirious
- Demented are more confused out of their environment especially at night ("sundowning").
- Fear is common. Be sensitive and allay their fears. Avoid question that may seem threatening to them.
- Need mental status exam.
- History may not reliable.
- Acutely Ill
- Need concise history and physical.
- May need to interview while doing exam.
- Finish interview after stable.
- Surgical
- Frightened even if calm appearance.
- Feel helpless and out of control.
- Lack of communication from surgeon makes worse.
- Depression if loss of body part.
- Allow time to release tension and feelings of loss during interview
- Alcoholic
- Feel castigated and alone. Alcohol is only friend.
- Often ready to talk and may have low self esteem.
- May be self destructive. May have fears of sexual inadequacy or homosexuality.
- Psychosomatic
- Psychological problems create physical ailments.
- May be unaware of emotional distress.
- Identify disorder, teach patient to cope with psych problems.
- Somatization is unconscious and patients are really suffering. Acknowledge their suffering is real. Never say problem is in your head.
- Use open ended questions to get insight.
- Dying
- Conscious of taking up doctor’s time and will start asking fewer questions.
- Don’t avoid dying patients because of own fears.
- Many fear process of dying more than death.
- May have anger or guilt or resentment.
- Envy healthy and deny imminent death.
- May deny disease even when asked directly.
- Most reach acceptance which may include apathy and withdraw.
- Dying patient needs to talk to someone.
- Appropriate response to an expression of grief may be period of silence.
- Disabled
Chapter 7
- Describe the “Four Principles of Physical Examination”, their importance, and clinical application.
- Four principles are inspection, palpitation, percussion, and auscultation.
- Describe what the examiner should observe while taking a history and how to apply clinically when evaluating a patient.
- General appearance: state of consciousness and personal grooming, distress? Groggy? Alert? Clean?
- State of nutrition: sunken eyes, temporal wasting, loose skin, thin, frail
- Body habitus:
- Asthenic: a condition of weakness, feebleness, or loss of vitality
- Ectomorphic characterized by a lean slender body build with slight muscular development
- Mesomorph: intermediate to asthenic and ectomorphic
- Hypersthenic or endomorphic: is short, round with good muscles, but weight problem
- Symmetry
- Posture and gait: foot drag? Shuffle?, limp?
- Speech: slurred? Appropriate words? Hoarse? High pitched?
- Apply the “preparations for the physical examination” clinically when evaluating a patient.
- Have all necessary equipment and place at bedside
- Close curtains for exam
- Wash hands – lather 10 seconds or use alcohol product in no visible soilage
- Have patient wear gown
- Do in order that requires least movement of patient
- Perform exam from right side of patient
- Expose only areas that are being examined at that time
- Continue speaking to patient during exam
- Discriminate which comments to refrain from when performing the physical examination.
- Avoid using "that's good", "normal", and "that's fine" as they may have unintended consequences with regard the pt's perception.
- Apply the precautionary guidelines for health-care workers from the CDC and OSHA and how to apply them when examining a patient.
- Use gloves when doing physical exam or handling blood soiled or body fluid sheets
- Wear gloves with patients with exudative lesions or weeping dermitis
- Use fluid resistant gowns, masks and eye covers when doing procedures
- Wash hands immediately if accidently soiled with blood or body fluids
- All sharps must be handled with care
- Don’t re-cap needles and dispose in puncture resistant containers
- Use mouthpieces for mouth to mouth
- Handle blood and body fluid samples with gloves
- Clean and decontaminant soiled surfaces with disinfectant
- Process reusable items according to recommendations
- If sharps injury or exposure to blood or body fluid clean area immediately and report
- All heath care workers should have Hep B vaccine
- Responsibility of health care worker not to transmit their disease to patient
Chapter 9
- Describe and recognize common symptoms of diseases involving the neck: neck mass and neck stiffness.
- Two most common physical findings are masses and stiffness.
- Interpret the signs and symptoms of diseases involving the neck: neck mass and neck stiffness.
- If there is associated pain with a mass in the neck, an acute infection is likely.
- Consider the age of the patient:
- Thyroglossal cyst occurs with patients under the age of 20, while thyroid disease occurs in older patients
- Consider the location of the mass:
- Lateral masses are more commonly neoplastic
- Midline masses are not associated with neoplasms but hyperplasia
- Superior masses correlate with head / neck tumors
- Inferior masses correlate with breast / stomach masses
- Neck stiffness is usually cause by spasm of the cervical muscles and commonly causes tension headaches.
- Depression is a common symptom of head and neck disease.
- Apply the components of the physical exam of the neck to a patient.
- No special equipment is required, and the patient is seated facing the examiner
- Inspection: position, scalp, masses, eyes, veins, nodularity
- Auscultation for carotid bruits
- Palpation: along muscles and major lymph node tracts using pads of fingers from posterior to anterior; thyroid gland
- Clinically correlate the symptoms and physical findings for the following disease processes: hyperthyroidism, hypothyroidism, thyroid nodules.
- Inspection:
- Proptosis: forward displacement of the eyes from thyroid dysfunction or orbital mass
- Thyromegaly: Graves’ disease causes bilateral proptosis and thyromegaly
- Thyroglossal duct cysts: are smooth, firm and midline
- Venous distention and nodularity may be associated with a goiter
- Palpation:
- Tender nodes are associated with inflammation, whereas firm nodes are associated with malignancy
- Thyroid
- Two methods for palpating the thyroid: anterior and posterior
- Rarely felt in it's healthy state.
- Hardness is associated with cancer or scarring
- Tenderness is associated with acute infections or hemorrhage
- Enlargement warrants auscultation
- A to-and-fro bruit of the superior pole highly suggests a toxic goiter
- Supraclavicular nodes: important; enlarged nodes can be felt with inspiration
- Inspection:
- Using the symptoms and / or physical exam findings pertaining to the neck, generate a diagnosis and a differential diagnosis.
- Grave’s Disease: proptosis, heat intolerance, hyperhidrosis, anxiety, insomnia, hyperpigmentation, palpitations, sweats, erythema, etc.
- Plummer’s Disease: toxic adenomatous goiter – frequently see atrial fibrillation
- Malignant thyroid nodule: male, one nodule, no FHx, change in voice, prior radiation for H/N
- Benign nodule: female, >1 nodule, FHx of benign thyroid disease, no voice change
- Hypothyroidism: weight gain, fatigue, chilly, lethargy
Chapter 10
- Describe the actions and innervations of the eye and extraocular muscles.
- Identify the major symptoms of eye disease.
- Interpret the symptoms of the major diseases of the eye and apply them clinically to a patient: loss of vision, eye pain, diplopia, tearing or dryness, discharge, and redness.
- Apply the components of the physical examination of the eye to a patient.
- Clinically correlate the symptoms and physical exam findings pertaining to the eye for the following disease processes: visual field defect, red eye (acute conjunctivitis, acute iritis, narrow-angle glaucoma, and corneal abrasion), diabetes, hypertension, and papilledema.
- Give a differential diagnosis based on symptoms and/or physical exam findings pertaining to the eye.
Chapter 11
Ear
- Describe the structure and innervations of the ear.
- Identify the major symptoms of ear disease and how these symptoms can identify diseases involving the ear: hearing loss, vertigo, tinnitus, otorrhea, otalgia, and itching.
- Interpret the symptoms of diseases of the ear and apply them clinically to a patient.
- Apply the components of the physical exam of the ear to a patient.
- Clinically correlate the symptoms and physical exam findings pertaining to the ear for the following disease processes: conductive and sensorineural hearing loss, otitis media. Serous otitis media, otitis externa, and vertigo.
- Generate a diagnosis and/or differential diagnosis based on symptoms and/or physical exam findings of the ear.
Nose
- Describe the structure of the nose.
- Illustrate how the major symptoms of nose diseases are used to identify nose diseases.
- Interpret the symptoms related to the nose and apply them clinically to a patient.
- Apply the components of the physical exam of the nose to a patient.
- Clinically correlate the symptoms and physical exam findings pertaining to the nose for the following disease processes: allergic rhinitis, sinusitis, and nonallergic rhinitis.
- Generate a diagnosis and/or differential diagnosis based on symptoms and/or physical exam findings of the nose.
Chapter 12
- Know the structures of the oral cavity and pharynx.
- Know the functions of the pharynx.
- Subdivisions: nasopharynx, oropharynx, hypopharynx.
- Fxn: provides swallowing, speech, and an airway.
- Know the important symptoms of disease of the oral cavity.
- Ulceration, bleeding, mass, halitosis, xerostomia (dry mouth).
- Apply the components of the physical exam of the oral cavity and pharynx to a patient.
- See cd.
- Clinically correlate the signs and symptoms of the following conditions:
- Aphthous ulcer
- Single canker sore. Most common acute oral ulcer.
- Relatively superficial w/ raised borders. On buccal or labial mucosa.
- Herpetic ulcer
- acute multiple ulcers, associated w/ vesicles.
- On mucocutaneous junction, hard palate, or gingivae.
- Crusting when bullae break.
- Chancre
- Painless, single lesion on lips or tongue.
- Lesion w/o central necrotic material.
- May have tender lymphadenitis.
- Squamous cell carcinoma:
- Single indurated sore on lips, tongue, mouth floor, or tongue (esp. on lateral borders)
- Erythroplakia of mouth floor and soft palate.
- Raised border, absence of necrotic material in crater.
- May have painless lymphadenopathy in neck.
- Candidiasis
- Burning tongue, inside of cheek or throat.
- Whitish pseudomembrane.
- Peeled off to reveal raw, red area that may bleed.
- Erythroplakia
- Painless, red area.
- Granular, red papules that bleed.
- Leukoplakia
- Painless, white area.
- Hyperkeratinized. Can’t be scraped off.
- Looks like flaking white paint. Often speckled w/ red spots.
- If associated with adenopathy, could be malignancy.
- Lipoma
- Painless mass on inner surface of cheek or tongue.
- Yellowish, soft, freely mobile.
- Lichen planus
- Usually no symptoms.
- Erosive form causes burning sores on inner cheeks and tongue.
- White reticulated papules bilaterally in lace-like pattern.
- Erosive form is hemorrhagic, ulcerated w/ possible white areas or bullae.
- May have pseudomembrane covering.
- Mucocele
- Intermittent painless swelling of lower lip, or inside cheek.
- Slightly bluish.
- Dome-shaped, freely-mobile cystic lesion.
- Hairy Tongue
- Gagging sensation.
- Large brown or black painless lesion on top of tongue.
- Elongation of filiform papillae and color change.
- Aphthous ulcer
Chapter 13
- Describe the topographical landmarks of the chest and utilize that knowledge to describe physical findings of the chest.
- Recognize the main symptoms of pulmonary disease and how these symptoms can identify disease.
- Interpret the symptoms of pulmonary disease and apply them clinically to a patient.
- Apply the components of the physical exam of the chest to a patient.
- Clinically correlate the symptoms and physical exam findings pertaining to the chest:
- Pulmonary Edema
- Pneumothorax
- Asthma
- Pneumonia
- Emphysema
- Pulmonary Embolism
- Pleural Effusion
- Generate a diagnosis and/or differential diagnosis based on symptoms and/or physical exam findings of the chest.
Chapter 17
- Describe the topographical landmarks of the abdomen and utilize that knowledge to describe physical findings of the abdomen.
- Recognize where abdominal structures are located by topographical quadrants of the abdomen.
- Recognize the main symptoms of abdominal disease and how these symptoms can identify disease.
- Interpret the symptoms of abdominal disease and apply them clinically to a patient.
- Apply the components of the physical examination of the abdomen to a patient.
- Clinically correlate the symptoms and physical exam findings pertaining to the abdomen.
- Generate a diagnosis and/or differential diagnosis based on symptoms and/or physical exam findings.